Chronic venous disease (CVD) is one of the most frequently treated conditions in the United States, and its most common symptom is varicose veins in the legs. But, like many patients, you may be wondering why your leg veins are raised, purple, and gnarled while the legs of those around you seem relatively unaffected. Though some inevitable changes happen in leg vasculature with age, varicose veins are widely considered to be among the most aesthetically displeasing. And, in many cases, they cause significant discomfort. So what are the root causes of varicose veins, and what can be done to get rid of them?
Dr. David Naar is Westlake, Ohio’s leading vein specialist. And at Premier Vein Clinic, he provides surgical management of CVD, varicose veins, spider veins, and reticular veins. As a board-certified vascular surgeon, Dr. Naar assesses the individual circumstances of each patient to create a personalized varicose vein treatment plan. Call (440) 641-0433 or fill out our online form to book a personal consultation, and say goodbye to your troublesome varicose veins with expert help!
Contents
About the Vascular System
The vascular system is an intricate network of blood vessels powered by nature’s most magnificent pump, the heart. This network of tubes carries oxygenated blood throughout the body, returning deoxygenated blood back to the heart. In the case of varicose veins, we are dealing with the peripheral vascular system, or PVS. The PVS is any blood vessel outside of the heart, which includes arteries (carrying blood away from the heart) and veins (carrying blood back toward the heart).
As with so many medical conditions, there are biological and environmental factors behind varicose vein development. The complex interactions between the heart, lungs, arteries, veins, and capillaries rely on every part of the system they are part of to function well. And, when the component parts of that system stop doing so, problems can occur.
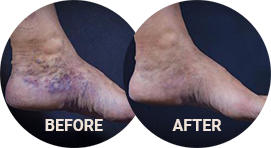
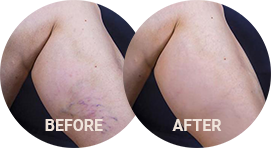
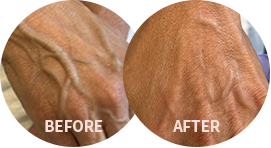
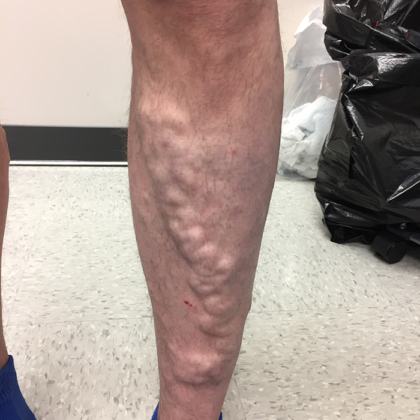
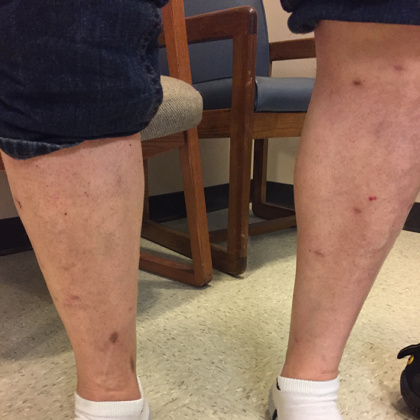
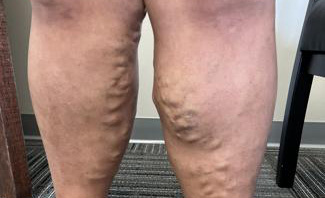
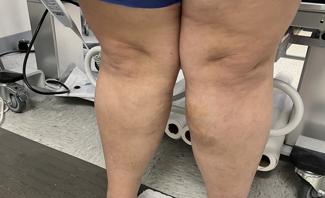
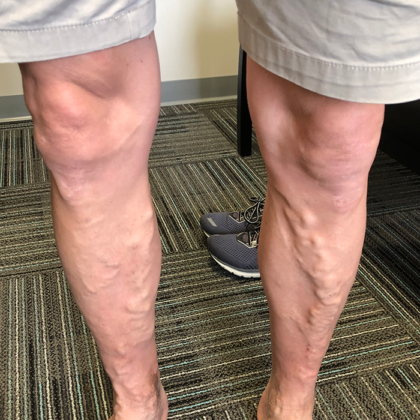
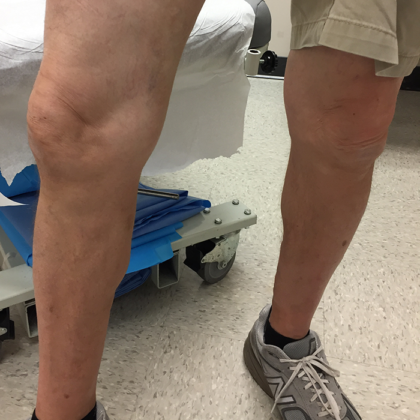
Before and After Photos
Signs of Varicose Veins
Varicose veins can develop in any vein close to the surface of the skin (superficial veins) and are most commonly found in the legs. The condition can involve one or multiple physiological signs, including the following.
- Raised, enlarged, “rubbery” veins
- Twisted vein appearance
- Purplish-blue/green coloration
- Itching or burning in the legs
- Leg cramps at night
- Swollen feet and ankles
- Feeling like you have “heavy” legs
- Aching, throbbing and cramping
- Dark discoloration of the ankles and legs
- Sores in the legs (venous ulcers)
Under Pressure
Veins function well in a low-pressure environment. Compared to the higher-pressure artery system, it deals with far larger volumes of blood. In fact, at any given point in time, nearly three-fourths of your blood volume is in your veins! (1) Within leg veins, muscle contractions and internal valves help to maintain the forward circulation of blood from the feet to the chest. But what if those valves were damaged?
How Did My Veins Get This Way?
If you have unsightly veins on your legs, there may be two culprits. Venous valves create seals at intervals along the vein, and are responsible for maintaining one-way blood flow back to the heart. But when they are physically damaged, and cannot form a complete seal, gravity wins and blood flows backwards. These poorly functioning valves, along with higher blood pressure in the legs, can lead to blood pooling. This is known as venous reflux.
Abnormal blood flow in both directions distorts the shape of the vein. It causes twists and bulges known as varicosities, which is why varicose veins often look so gnarled. Left untreated, venous reflux contributes further to CVD and a worsening of backflow called chronic venous insufficiency (CVI).
As any varicose vein patient will tell you, without treatment, varicose veins will only get worse over time. Although precise numbers are difficult to obtain, data suggests that CVD prevalence is between 60 and 80% worldwide, (2) causing many thousands of people to seek treatment every year.
Risk Factors
There are intrinsic (internal) and extrinsic (external) factors in varicose vein development. These include the following.
Family History
Susceptibility to many diseases has a genetic basis, and data shows that venous disease is no exception. If your relatives have varicose veins and/or CVD, there’s a higher likelihood you will develop them too. By studying thousands of DNA samples, researchers have so far identified 30 genetic markers associated with varicose veins. Interestingly, the same large-scale study showed that taller people were more susceptible to venous disease. (3)
Increased Age
Older people are more susceptible to varicose vein development due to vein tissues becoming weaker, decreased mobility, and illness. In particular, an age-related decrease in muscle tone in the calf can worsen valve function. The risk of developing deep vein thrombosis (DVT), a related vascular condition that can cause blood clots, also increases significantly with age. (4)
Female Sex
Women are more likely to develop varicose veins. Early signs of venous reflux occur in around 25% of women and 15% of men. During pregnancy, hormone changes can negatively affect valve efficiency and cause venous walls to thin. (5)
Multiple Pregnancies
Pregnancy puts enormous strain on the body. Increased levels of the hormone progesterone, pressure on the pelvic veins, and a subsequent increase in leg vein blood pressure all contribute to higher varicose vein risks for pregnant women. Women who have had been pregnant before are more likely to develop them than women who have never been pregnant, and women who have had multiple pregnancies are at the highest risk. (6)
Standing or Sitting for Long Periods
We all know that staying active is a key factor in maintaining our long-term health goals. Certain professions that require extended periods of standing, or prolonged periods of sitting, lead many patients to become more likely to develop varicose veins. One study showed that prolonged standing in particular accounts for more than one in five of all varicose vein-related hospital admissions in working-age patients. (7)
Obesity
A higher body mass index (BMI) is associated with varicose vein risks because of the associated strain on the circulatory system. Clinical data suggests varicose veins may develop as a result of elevated testosterone levels, and higher hip and thigh circumferences in post-menopausal women. (8)
Deep Vein Thrombosis
Diseases of the same system are often linked, and the same can be said for DVT and varicose veins. Although it’s not completely clear if one condition precedes the other, or vice versa, researchers agree that they share a common set of risk factors. (9)
If varicose veins are making your life difficult, find relief with professional treatment at Premier Vein Clinic! Start by making an appointment with board-certified vascular surgeon Dr. David Naar.
Varicose Vein Treatment
Ambulatory Phlebectomy for Varicose Veins
Considered along with RF ablation, the most effective treatment method for varicose veins, ambulatory phlebectomy removes the problem vein permanently via small incisions in the leg. By taking sections of the vein out at different points on the leg, the entirety of the structure is removed. During this process, the circulatory system immediately reroutes blood flow back to the heart via other blood vessels. The cosmetic and functional results of micro-phlebectomy are outstanding.
Radio Frequency Venous Ablation
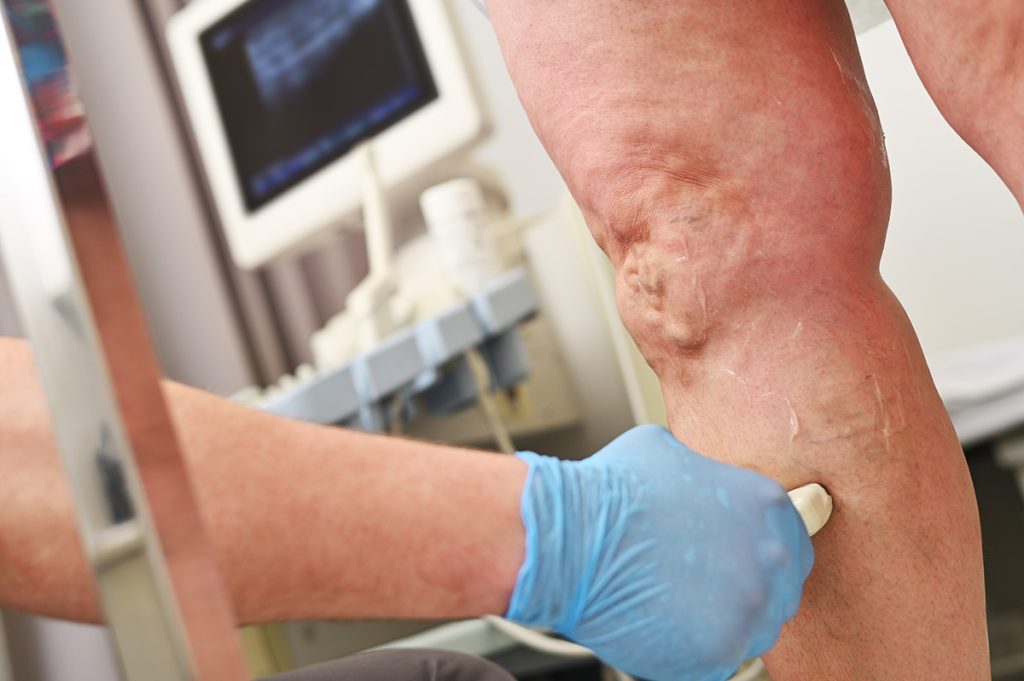
RF ablation is an effective, minimally-invasive way to remove varicose veins. Dr. Naar uses ultrasound to guide a slim catheter through the vein, through which he places a micro fiber optic cable. As the cable emits radio frequency thermal energy as heat, the vein shrivels and collapses in on itself.
Endovenous Chemical Foam Ablation
Endovenous chemical foam ablation is similar to RF ablation, but instead of using RF energy, it uses a chemical irritant inside the vein to weaken structures and destroy it. This micro-foam, called sclerosant, is beneficial for patients with both varicose veins and spider veins. What’s more, this non-surgical method results in minimal scarring and superb esthetics.
Cost of Varicose Vein Treatment in Westlake, OH
The cost of your vein treatment will depend on the details of your personalized treatment plan, which will be expertly created by Dr. Naar. If you have questions about venous disease, read our helpful patient education page. Once you’re ready to book your consultation at Premier Vein Clinic, please call (440) 641-0433 or fill in our online inquiry form.
Read Dr. Naar’s blog for more details about the most effective varicose vein treatments.
References
- Tucker WD, Mahajan K. Anatomy, Blood Vessels. Nih.gov. Published January 4, 2019. https://www.ncbi.nlm.nih.gov/books/NBK470401/
- Ortega MA, Fraile-Martínez O, García-Montero C, et al. Understanding Chronic Venous Disease: A Critical Overview of Its Pathophysiology and Medical Management. Journal of Clinical Medicine. 2021;10(15):3239. https://doi.org/10.3390/jcm10153239
- Fukaya E, Flores AM, Lindholm D, et al. Clinical and Genetic Determinants of Varicose Veins. Circulation. 2018;138(25):2869-2880. doi:10.1161/circulationaha.118.035584 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6400474/
- Molnár AÁ, Nádasy GL, Dörnyei G, et al. The aging venous system: from varicosities to vascular cognitive impairment. GeroScience. 2021;43(6):2761-2784. doi:10.1007/s11357-021-00475-2 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8602591/
- Antani MR, Dattilo JB. Varicose Veins. PubMed. Published 2022. Accessed November 29, 2022. https://www.ncbi.nlm.nih.gov/books/NBK470194/#:~:text=Varicose%20veins%20are%20seen%20globally
- Smyth RM, Aflaifel N, Bamigboye AA. Interventions for varicose veins and leg oedema in pregnancy. The Cochrane Database of Systematic Reviews. 2015;2015(10). doi:10.1002/14651858.CD001066.pub3 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7050615/
- Tuchsen F. Prolonged standing at work and hospitalisation due to varicose veins: a 12 year prospective study of the Danish population. Occupational and Environmental Medicine. 2005;62(12):847-850. doi:10.1136/oem.2005.020537 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1740939/
- Iannuzzi A, Panico S, Ciardullo AV, et al. Varicose veins of the lower limbs and venous capacitance in postmenopausal women: Relationship with obesity. Journal of Vascular Surgery. 2002;36(5):965-968. doi:10.1067/mva.2002.128315 https://www.jvascsurg.org/article/S0741-5214(02)00264-1/pdf
- Chang SL, Huang YL, Lee MC, et al. Association of Varicose Veins With Incident Venous Thromboembolism and Peripheral Artery Disease. JAMA. 2018;319(8):807. doi:10.1001/jama.2018.0246 https://jamanetwork.com/journals/jama/fullarticle/2673551