Stasis Dermatitis
Conveniently located to serve the areas of Westlake, OH

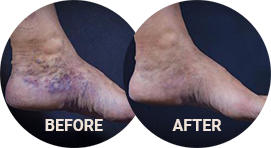
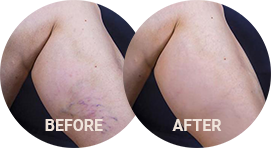
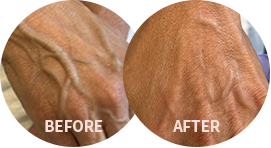
Stasis dermatitis, also known as venous eczema or gravitational dermatitis, is a condition where inflammation and redness of the skin occurs in the lower legs due to poor functioning veins. It is often triggered by long periods of standing or sitting, and the underlying cause is typically varicose veins. This condition can lead to uncomfortable symptoms such as itching, burning, and dry, scaly skin.
Although research is not conclusive, an estimated 15 to 20 million patients over age 50 in the United States suffer from the condition. (1) However, there are treatments that can help to relieve the stress and discomfort, including the treatment of varicose veins via endovenous ablation, sclerotherapy, or ambulatory phlebectomy.
At Premier Vein Clinic, board-certified vascular surgeon Dr. David Naar can help you find relief from stasis dermatitis. To book your one-on-one consultation with him at his Westlake, OH location, call (440) 641-0433 or use the simple form on our website to get in touch regarding your appointment.
Contents
About Stasis Dermatitis
Stasis dermatitis is an inflammatory skin disorder caused by poor circulation in the veins of the lower legs, known as venous reflux. This condition is more commonly found in elderly individuals, and in women, but it can affect anyone.
What is Venous Reflux?
When the valves in the veins become weak or damaged, they are unable to adequately circulate blood from the legs back to the heart. This causes blood to pool in the veins of the lower legs and increases the pressure in the veins. This increased pressure can lead to swelling and inflammation of the skin and tissues, resulting in stasis dermatitis.
Symptoms of Stasis Dermatitis
The most common symptom of stasis dermatitis is an itchy rash on the lower legs. This rash is usually red, scaly, and may be accompanied by swelling and pain. Additional symptoms include:
- Dryness
- Thickening of skin
- Darkening of skin
- Crusting and bleeding
- Ulcers
Is My Diagnosis Correct?
Stasis dermatitis is a skin condition that is often misdiagnosed. Conditions similar to it include the following. (2)
Cellulitis
Cellulitis is a bacterial skin infection that can develop when bacteria enters the skin through cuts, scrapes, or insect bites. It is most commonly caused by staphylococcus and streptococcus bacteria, although other types of bacteria can also lead to cellulitis. Cellulitis can occur anywhere on the body but is most common on the lower legs due to their proximity to the ground.
Contact Dermatitis
Contact dermatitis is a type of eczema that affects the top layer of the skin. It usually develops within minutes to hours after contact with an allergen or irritant. The symptoms of contact dermatitis vary from person to person, but generally include itching, redness, and swelling. In some cases, blisters may form and break open, leaving behind weeping sores. The affected skin may also become scaly and dry.
Pigmented Purpuric Dermatoses
Pigmented purpuric dermatoses (PPD) is a group of skin conditions that causes red-brown discoloration of the skin. PPD can occur anywhere on the body, but it is most commonly seen in the lower legs. It is often caused by an underlying condition such as varicose veins, infection, or ulcerations. If you are experiencing any symptoms of PPD, it is important to seek medical care from a specialist as soon as possible.
Receive a conclusive diagnosis from Dr. Naar by booking a personal consultation at Premier Vein clinic.
The CEAP Classification System
Venous conditions are assessed by a vascular surgeon. Stasis dermatitis can be graded using the Clinical Etiology Anatomy Pathophysiology (CEAP), a classification system for venous disorders. (3)
- C0: No visible or palpable signs of venous disease
- C1: Telangiectasias or reticular veins present
- C2: Varicose veins present
- C3: Edema (swelling)
- C4: Changes in skin and subcutaneous tissue secondary to chronic vein disease
- C5: Healed venous leg ulcer
- C6: Venous leg ulcer
Stasis dermatitis is classified as C4 on the CEAP scale.
How Can Treatment Improve Stasis Dermatitis?
Dr. Naar understands that stasis dermatitis can cause severe discomfort, which is why his goal is to provide relief and restore optimal health to your legs. Here are some of the benefits you can expect after your treatment:
- Improved circulation
- Reduced inflammation
- Alleviated itching and burning
- Smoother, healthier-looking skin
- Relief from pain
- Reduced risk of complications such as ulcers
Help for Stasis Dermatitis
At Premier Vein Clinic, Dr. Naar will assess your individual situation and develop a personalized treatment plan to relieve your symptoms. Treatment for stasis dermatitis typically involves lifestyle changes, medications, and/or surgical procedures.
Lifestyle Changes
Lifestyle changes may include elevating the lower legs when resting, avoiding long periods of standing or sitting, and weight management.
Compression Therapy
Compression therapy helps reduce swelling and improve circulation. Compression stockings are worn over the affected area to apply pressure and help keep fluid from pooling in the lower legs. These stockings come in a variety of sizes and materials, so they can be customized to fit your needs.
Medications
Topical creams and ointments may be prescribed to reduce inflammation and itching. Oral medications may also be prescribed to reduce inflammation.
Minimally-Invasive Surgery
In severe cases, surgery may be recommended to treat underlying varicose veins. There are several different types of procedures that can be used to address varicose veins.
Living with varicose veins is hard enough without the stress of secondary conditions that develop because of them. Call Westlake’s Premier Vein Clinic at (440) 641-0433 or complete an inquiry form to find treatment for stasis dermatitis.
In-Office Varicose Vein Treatments
Dr. Naar designs individualized treatment plans to improve the appearance and health of your legs. Minimally-invasive treatments at Premier Vein Clinic are safe and effective, with minimal, if any, downtime.
Radiofrequency Ablation
For those suffering from stasis dermatitis due to varicose veins, radiofrequency ablation may be recommended. Ablations are performed under local anesthesia and involve inserting a small catheter into the vein. The catheter delivers radiofrequency energy energy to the area, which causes the vein wall to heat up and collapse, improving circulation and relieving symptoms.
Endovenous Chemical Foam Ablation
Endovenous chemical foam ablation is a minimally invasive, non-surgical procedure that is used to treat varicose veins and other vein issues. During the procedure, a catheter is inserted into the affected vein and a solution of sclerosant foam is injected. The foam works by causing inflammation in the vein, which causes it to close off and eventually disappear.
Ambulatory Phlebectomy
Ambulatory phlebectomy is a safe and effective treatment option for varicose veins. During the procedure, Dr. Naar will make a series of small incisions in the leg. Through these incisions, he will use a special tool to remove the damaged veins. The entire process is performed using local anesthesia and takes about 1-2 hours. After the procedure, you may experience some mild discomfort and bruising, but there is no need for extensive bed rest. Most patients can resume normal activities within one to two days.
Sclerotherapy
Sclerotherapy is an injection-based treatment used to treat spider veins and smaller varicose veins. During the procedure, a sclerosing agent is injected directly into the vein, causing it to collapse and eventually fade from view. This procedure is fast, safe, and effective.
Personal Consultation
The first step in treating stasis dermatitis is to meet with Dr. Naar for a personal consultation at our Westlake office. During this appointment, we will review your medical history and discuss your symptoms. We will then assess the condition of your legs and determine if there are any underlying issues that are contributing to your condition. This allows us to develop a personalized treatment plan tailored to your individual needs.
Cost of Stasis Dermatitis Treatment in Westlake, OH
Stasis dermatitis can be a frustrating condition to live with, but there is hope. At Premier Vein Clinic, our goal is to provide personalized care that is tailored to each patient’s unique needs. If you are suffering from stasis dermatitis, we invite you to contact us for an appointment today by calling (440) 641-0433. We look forward to helping you find relief!
FAQ
How do I prevent stasis dermatitis?
While anyone can develop stasis dermatitis, there are steps you can take to reduce your risk. Regular exercise can help improve circulation, and wearing compression stockings can help relieve symptoms. Elevating your legs above your heart for 15 minutes several times a day can also help reduce swelling and inflammation. Eating a balanced diet, quitting smoking, and maintaining a healthy weight can also help.
What happens if I leave stasis dermatitis untreated?
If left untreated, stasis dermatitis can lead to more serious problems such as infection and skin ulceration. In extreme cases, these ulcers can become deep and infected. They can even cause permanent damage to the skin and tissue. It’s important to seek treatment as soon as possible to avoid any serious complications.
Is there a cure for stasis dermatitis?
Unfortunately, stasis dermatitis cannot be cured. However, with proper treatment, its symptoms can be managed and the condition kept under control. Treatment typically includes lifestyle changes, medications, and procedures like endovenous ablation and sclerotherapy.
References
- Filit HM 2010, Rockwood K, Woodhouse K. Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. ScienceDirect. Published 2010. Accessed March 10, 2023. https://www.sciencedirect.com/book/9781416062318/brocklehursts-textbook-of-geriatric-medicine-and-gerontology
- Sundaresan S, Migden MR, Silapunt S. Stasis Dermatitis: Pathophysiology, Evaluation, and Management. American Journal of Clinical Dermatology. 2017;18(3):383-390. doi:https://doi.org/10.1007/s40257-016-0250-0
- Lurie F, Passman M, Meisner M, et al. The 2020 update of the CEAP classification system and reporting standards. Journal of Vascular Surgery: Venous and Lymphatic Disorders. 2020;8(3):342-352. doi:https://doi.org/10.1016/j.jvsv.2019.12.075