Skin Discoloration & Damage
Conveniently located to serve the areas of Westlake, OH

A change in the pigmentation or texture of skin in the lower legs is often an indicator of venous disease. Skin discoloration and damage can occur in any part of the body, though it is commonly found on the lower legs and ankles in patients with chronic venous conditions. Chronic venous insufficiency (CVI), a condition where the veins fail to efficiently return blood to the heart, can contribute to the formation of varicose veins and other complications.
There are also various stages of chronic venous disease (CVD) which are characterized by a progressive worsening of varicose veins, particularly in the lower extremities. These skin conditions can cause physical and mental discomfort for the sufferer and may also be resistant to treatment without specialized intervention.
At Premier Vein Clinic in Westlake, experienced vascular surgeon Dr. David Naar provides treatments that can help patients to manage skin conditions caused by venous disease. To book a consultation to discuss varicose veins and their related skin conditions, call (440) 641-0433 or complete a short form for more details.
Contents
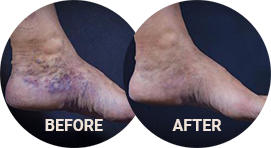
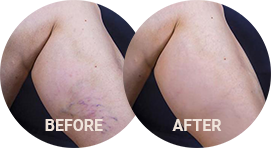
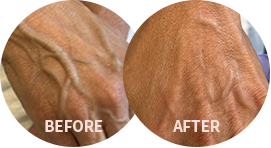
Before and After Photos
About the Peripheral Venous System
The peripheral venous system’s function is to transport blood back to the heart. However, if these structures are damaged or in poor health, they can fail to function as they should. Venous disease develops when the pressure inside the vein is too great and blood cannot return to the heart efficiently. This can occur due to: (1)
- Valvular Incompetence – The valves that open and close to facilitate blood flow stop working efficiently, causing venous reflux.
- Thrombotic or Non Thrombotic Blockage – Blood clots or other debris can hinder blood flow.
- Extrinsic Compression – Extrinsic compression occurs when surrounding structures affect a vein’s ability to work optimally in tight anatomic spaces.
Varicose veins and spider veins are among the most common manifestations of venous disease. These enlarged, twisted veins often appear on the legs and can cause discomfort, pain, and aesthetic concerns.
Classification of Venous Disease
CVD can be measured using 7 clinical categories. (2)
- C0: No visible or palpable signs of venous disease
- C1: Telangiectasies or reticular veins
- C2: Varicose veins (diameter of 3mm or more)
- C3: Edema (swelling)
- C4: Changes in skin and subcutaneous tissue secondary to CVD
- C4a: Pigmentation or eczema
- C4b: Lipodermatosclerosis or atrophie blanche
- C5: Healed venous ulcer.
- C6: Active venous ulcer.
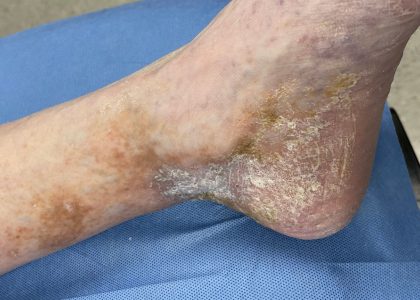
Skin Discoloration & Damage from Venous Disease
Hyperpigmentation
Chronic venous disease can lead to hyperpigmentation, which is the darkening of the skin in affected areas. The discoloration can vary from mild to severe. This occurs due to the accumulation of blood byproducts in the tissues. The skin may appear brownish or reddish in color.
Venous Eczema
Also known as gravitational dermatitis, venous eczema is a type of skin inflammation that occurs due to poor blood circulation in the legs. It can cause redness, itching, scaling, and even oozing blisters.
Lipodermatosclerosis
Lipodermatosclerosis is the hardening and inflammation of the fatty tissue under the skin. It can cause pain, tenderness, and changes in skin texture, such as thickening and hardening. Common risk factors for developing lipodermatosclerosis include: (3)
- Obesity
- Age
- A family history of venous insufficiency
- A prior history of deep vein thrombosis (DVT)
- Tobacco use
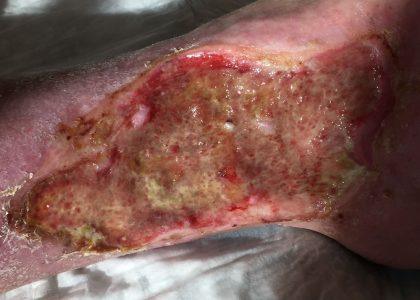
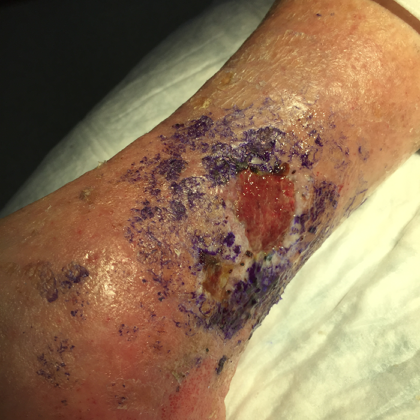
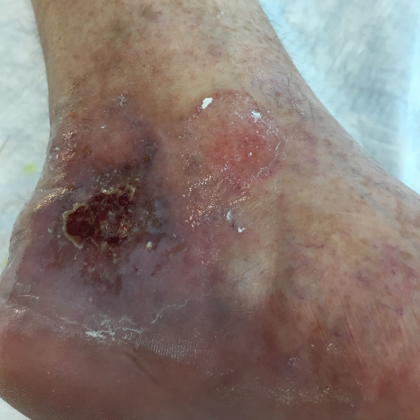
Venous Ulcers
As venous disease progresses, it can result in the development of venous ulcers. These open sores typically occur around the ankles and are often painful and slow to heal. Proper diagnosis and management are crucial to prevent complications and promote healing. Atrophie blanche, or scarring that can occur after a venous ulcer has healed, can appear as mottled white marks on the skin.
Read more about what causes venous ulcers on our blog.
Venous Stasis Dermatitis
Stasis dermatitis is a condition characterized by skin inflammation, discoloration, and dryness, primarily affecting the lower legs. It occurs when blood pools in the veins and impairs the delivery of nutrients to the skin cells.
Cellulitis
In severe cases of venous disease, the compromised skin barrier can allow bacteria to enter and cause a serious infection known as cellulitis. Symptoms include redness, warmth, pain, and swelling in the affected area.
Preparing for Vein Treatment
Before undergoing any treatment for venous disease and its related skin conditions, it is crucial to be well-prepared. At Premier Vein Clinic, our goal is to ensure that you have all the necessary information and resources to make your experience as smooth and successful as possible.
Compression Stockings
These specialized stockings are an important aspect of managing venous disease. Prior to your treatment, we will provide you with detailed instructions on how to properly wear and care for your compression stockings.
Ultrasound Imaging
Before proceeding with any treatment, we will conduct thorough ultrasound imaging to accurately diagnose and assess the extent of your condition. This allows us to tailor the treatment plan specifically to your needs.
Anticoagulant Medications
In some cases, anticoagulant medications may be prescribed to prevent blood clots or manage other underlying conditions. It is important to follow the prescribed dosage and frequency as instructed by our medical team.
Surgical Dressings
If you require any surgical interventions, such as wound debridement or ulcer treatment, appropriate surgical dressings will be applied to facilitate healing and prevent infection. We will provide you with detailed instructions on how to care for these dressings at home.
Skin Barrier Creams
For individuals with compromised skin integrity, such as those with venous ulcers, skin barrier creams can help protect the skin and promote healing. Our team will guide you in selecting the most suitable barrier cream for your condition.
Wound Healing Ointments
Depending on the severity of your skin condition, we may prescribe specialized wound healing ointments to facilitate the healing process and minimize scarring. These ointments should be applied as directed by our medical team.
Vein Health Procedures
To facilitate skin healing, it is vital to treat venous disease. There are a number of methods of doing so.
Sclerotherapy
Sclerotherapy is a highly effective and minimally invasive procedure designed to treat varicose veins, spider veins, and other forms of venous insufficiency. It involves injecting a special solution directly into the affected veins. This solution irritates the lining of the vein, causing it to collapse and eventually be resorbed by the body. Over time, the treated veins fade away, leaving behind clearer, healthier-looking skin.
Ambulatory Phlebectomy
Ambulatory phlebectomy involves the removal of varicose veins through small incisions made in the skin. Unlike vein stripping, which requires general anesthesia and a hospital stay, this procedure can be performed in our Westlake clinic using local anesthesia. It is a well-tolerated medical procedure that allows patients to return home on the same day, resuming their daily activities without extensive downtime.
Radiofrequency Venous Ablation
Radiofrequency venous ablation involves inserting a catheter into the affected vein under local anesthesia. The catheter emits radiofrequency energy that heats and seals the vein, effectively closing it off. This heat-based vein closure method allows for improved blood flow redirection through healthier veins. Treatment requires only a small incision, resulting in minimal scarring. Patients typically experience immediate relief from their symptoms and notice a significant improvement in the appearance of their legs over time.
Endovenous Chemical Foam Ablation
Endovenous chemical foam ablation involves the use of a specialized foam solution that is injected directly into the affected veins. The foam serves two purposes: it displaces the blood within the vein, allowing for better contact between the solution and the vein walls, and it irritates the inner lining of the vein, causing it to collapse and eventually be resorbed by the body. It is a minimally invasive procedure that can be performed on an outpatient basis, meaning no hospital stay is required. The foam solution allows for precise targeting of the affected veins, resulting in more efficient treatment and faster recovery times. Additionally, because the procedure does not involve any surgical incisions, scarring is minimal or non-existent.
Cost of Varicose Vein Treatment in Westlake
At Premier Vein Clinic, your satisfaction and well-being are our top priorities. We are here to answer any questions you may have about the cost of endovenous chemical foam ablation or any other aspect of your vein treatment journey. Contact us today at (440) 641-0433 to take the first step towards healthier, more beautiful legs.
FAQ
Why is the skin on my ankles so sore near my varicose veins?
If you have a condition such as venous insufficiency, you may experience itchy, textured skin on the legs and ankles. This can develop into eczema and even venous ulcers if left untreated. It is essential to consult with a board-certified vascular surgeon promptly and receive effective treatment for vein-related skin conditions.
If I get my varicose veins treated, will my skin conditions get better?
Patients who have vascular conditions with related skin problems can find relief with non-surgical and minimally invasive vein treatments to improve their skin and restore comfort.
Why won’t my venous ulcers heal?
Patients who have vascular conditions with related skin problems can find relief with non-surgical and minimally invasive vein treatments to improve their skin and restore comfort.
References
- Singh A, Zahra F. Chronic Venous Insufficiency. PubMed. Published 2023. Accessed October 24, 2023. https://www.ncbi.nlm.nih.gov/books/NBK587341/#:~:text=Persistent%20venous%20hypertension%20can%20result
- Zegarra TI, Tadi P. CEAP Classification Of Venous Disorders. PubMed. Published 2022. https://www.ncbi.nlm.nih.gov/books/NBK557410/
- Geist RS, Crane JS. Lipodermatosclerosis. PubMed. Published 2023. https://www.ncbi.nlm.nih.gov/books/NBK594262/