Treating vascular issues such as spider veins is usually a cosmetic endeavor. Telangiectasias, the medical term given to spider veins and larger reticular veins, are small broken blood vessels near the surface of the skin. These vessels can appear in the lower extremities. They are usually no bigger than 1.0 mm (0.04 in) in diameter. However, despite the fact that spider veins are not in and of themselves a cause for major concern, their presence may indicate that there are further underlying problems with the vascular system that need treatment.
Westlake’s Premier Vein Clinic is a specialized center for the treatment of varicose veins, spider veins, reticular veins, and other venous conditions. Dr. David Naar uses his years of experience as a Board Certified Vascular Surgeon to help his patients address troublesome veins for cosmetic and medical reasons. Take the first step toward removing your spider veins by calling (440) 641-0443 or by filling out our online form.
Contents
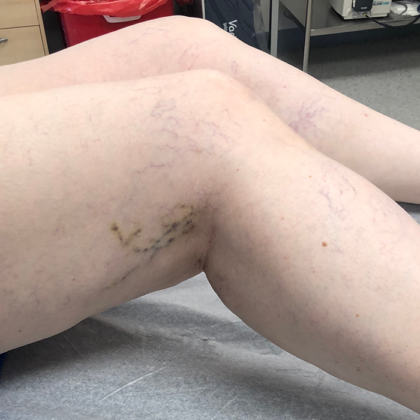
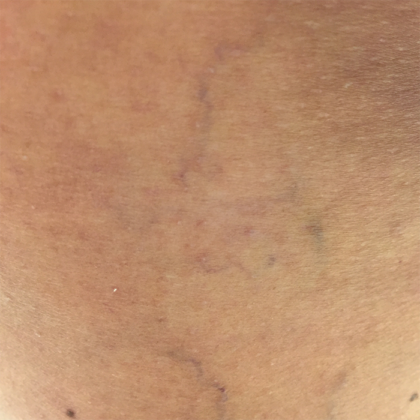
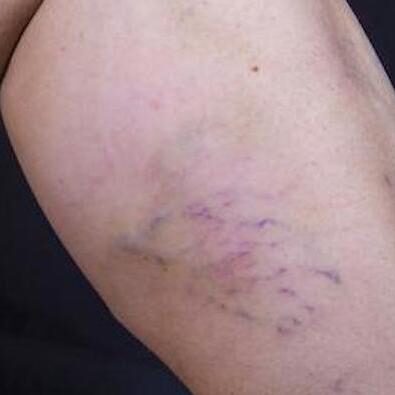
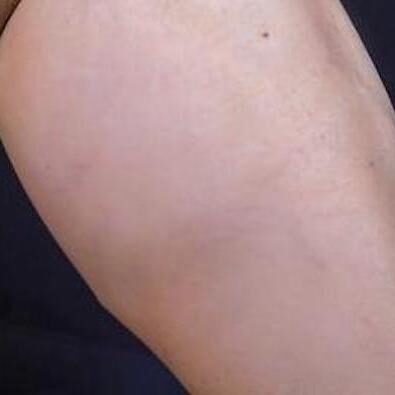
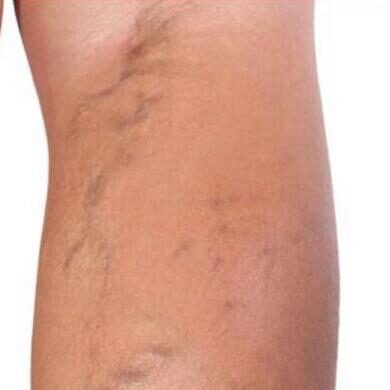
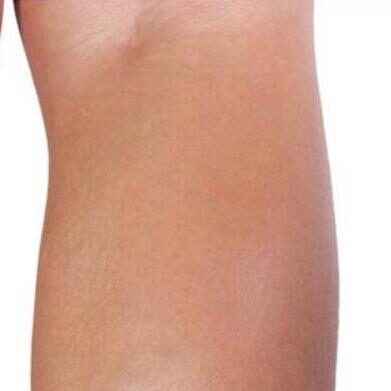
Before & After Photos
Before and After Photos
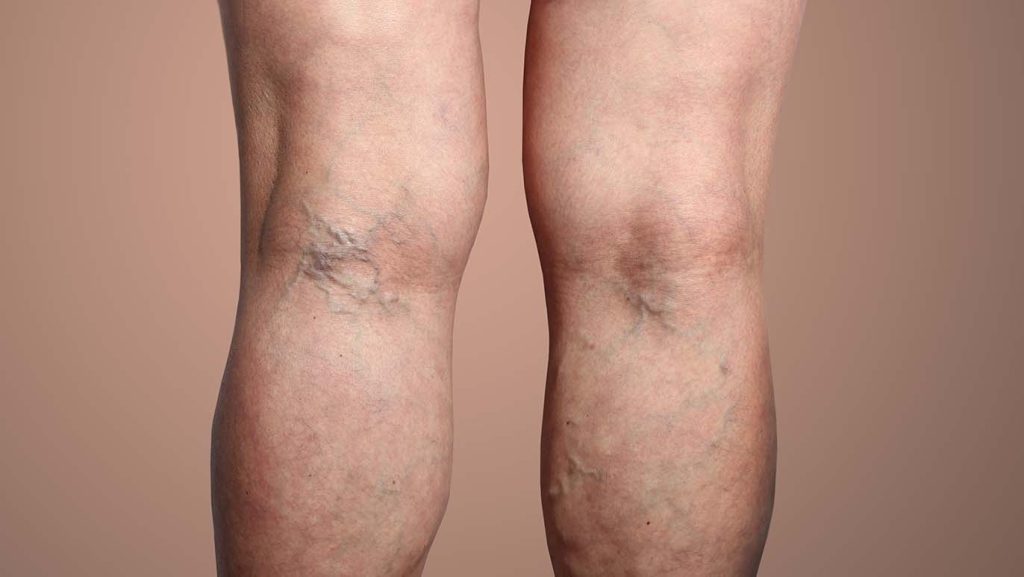
About Spider Veins
Spider veins are thin red, blue, or purple strand-like lines that are visible close to the outermost layer of the skin. These lines bulge and branch out from a central point resulting in a spider-like appearance. (1) Spider veins are usually much thinner than varicose veins. They usually appear as more jagged shapes under the skin and share many features of reticular veins, another type of telangiectasia. Reticular veins are larger than spider veins and are usually less than 3 mm (0.19 in). One, two, or all of these conditions may be present simultaneously in a particular area.
Small clusters of telangiectasias can appear and multiply over time. They can be present on the feet, ankles, legs, face, and the backs of the knees. And, for some patients, their appearance can cause self-consciousness and embarrassment. Patients may hide their legs underneath pants or leggings, limiting clothing choices. There are various treatments for the removal of spider veins. One of the most effective ways to rid yourself of spider veins is sclerotherapy; the injection of a solution into these structures that shrinks them and eventually renders them invisible.
Varicose Veins
Many physicians consider spider veins and reticular veins to be the first stage in the development of venous disease; which may lead to varicose veins. If spider veins are present, this could indicate other vascular problems, particularly varicose veins. Varicose veins are thick, ropy structures that may bulge out of the skin. They are usually purplish blue in color and can twist in river-like undulations along the backs of the legs, thighs, calves, ankles, and feet. There are many symptoms patients can experience due to varicose veins, including:
- Leg Pain
- Cramping
- Leg heaviness
- Aching
- Swollen Feet and Ankles
- Throbbing Pain
- Itchy, Dry Skin
- Skin Discoloration
- Burning
- Numbness, tired legs.
Complications from Varicose Veins
Left untreated, varicose veins can cause further complications, including significant swelling of the affected area (edema), skin damage and darkening, mobility issues, and lesions known as venous ulcers that can cause serious disability, pain and suffering. (2) If varicose veins are causing you discomfort, please discuss solutions such as radiofrequency laser ablation and endovenous chemical foam ablation with Dr. Naar.
What Causes Spider Veins and Varicose Veins?
The cardiovascular system transports blood throughout the body. Deoxygenated blood must be returned to the heart for reoxygenation. Our veins direct blood flow back to the heart, but sometimes, they can become damaged. Inside every vein there are small one-way valves. These valves prevent the backflow of blood.
When these valves are not working correctly, they fail to create a seal when they close, and blood can flow backwards and pool, causing structural changes. Spider veins, reticular veins, and varicose veins can materialize due to faulty valve function, which is a condition known as venous reflux, or venous incompetence.
Should I Treat My Spider Veins?
Though many spider veins are asymptomatic, they may indicate an underlying problem with your circulatory system. Research suggests that the presence of telangiectasias is strongly linked to chronic venous insufficiency (CVI). CVI is a progressive, ongoing malfunction of venous valves.
A patient can have problems with superficial veins (those closer to the skin’s surface), or deeper veins (those closer to the center of the leg). Perforating veins connect deeper veins with superficial veins. Approximately 50% to 62% of insufficient perforating veins are found where telangiectasias are present. (3) This evidence strongly suggests a link between spider veins and the eventual development of more serious venous disease.
Assessing Venous Disease
The CEAP system is used to assess the severity of venous insufficiency. CEAP classification stands for Clinical (C), Etiological (E), Anatomical (A), and Pathophysiological (P). The clinical severity of the vein is measured in the following way:
C0: No visible or palpable signs of venous disease
C1: Spider veins and reticular veins are present
C2: Varicose veins over 3 mm are present
C3: Area is swollen (edema)
C4: Changes in skin and subcutaneous tissues
C5: Healed venous ulcer
C6: Active venous ulcer (4)
Benefits of Sclerotherapy
Benefits of sclerotherapy include:
- In-office short treatment duration
- Relief from unsightly veins
- Low-risk minimally-invasive procedure
- Immediately noticeable results
- May improve self-confidence
- Allows for broader clothing choices
The choice to undergo vein treatment is a personal one. Depending on your circumstances, if you choose not to undergo sclerotherapy early on, you may face problems with your leg veins later in life, and an increased likelihood of developing varicose veins and further venous insufficiency.
Sclerotherapy is the most common way to eliminate spider veins. It’s a good treatment option for patients with unsightly veins in the feet and legs. If you have spider veins and varicose veins, you may consider this treatment. By injecting a solution called sclerosant into the vein, the treatment irritates the structure and closes it off. Blood flow redirects to other veins in the area, and over time, the vein debris is reabsorbed by the body. (4)
Candidates for Sclerotherapy
Vascular surgeons consider sclerotherapy to be a first-line treatment for spider veins on the legs. (1) Patients can undergo cosmetic or medical sclerotherapy for the removal of spider veins. Where the procedure is performed for cosmetic reasons, the patient is looking to change the aesthetic appearance of the area only. Where there is pain or itching, which would be more common in later-stage venous insufficiency, medically classified sclerotherapy is appropriate. You may not be a good candidate for sclerotherapy if you:
- Have an active infection in the treatment area
- Have severe arterial disease
- Have been diagnosed with deep venous thrombosis (DVT)
- Are pregnant (5)
Women who have recently given birth should wait at least 3 months after their delivery before undergoing sclerotherapy treatment.
Personal Consultation
Dr. Naar will assess your problem veins at your personal consultation. During your visit with us, we will ask you to fill out our patient intake forms. These forms will ask you to provide some details about your medical history, including any problems you have with your cardiovascular system. Dr. Naar will visually inspect your areas of concern and determine whether spider veins, reticular veins, varicose veins, or multiple indications of venous disease are present. If you are a suitable candidate for treatment, he will explain the details of the sclerotherapy procedure and schedule your treatment date.
If more than one sclerotherapy session is required, you can discuss the scheduling of multiple treatment appointments. In some but not all cases, patients who are treating spider veins also have varicose veins they want to remove. Dr. Naar will create a treatment plan that allows for all areas of concern to be addressed.
Sclerotherapy Procedure
After applying a topical numbing gel, the sclerotherapy procedure begins. Using ultrasound, Dr. Naar examines the treatment area for venous obstruction and venous reflux/incompetence. He will identify abnormal blood flow pathways and mark the target vessels for injection. Dr. Naar injects a sclerosing agent, a type of detergent, into each problem vein to close it shut. This agent can be in liquid or foam form. He carefully injects the solution using a very fine needle (30 gauge), guided by ultrasound. (1)
Results
Patients notice the early results of sclerotherapy immediately after their treatment. Dr. Naar will ask you to follow written aftercare directions, and you will need to wear compression stockings to direct blood flow efficiently. Sclerotherapy is the gold standard treatment for spider and reticular veins, rendering them virtually invisible and gradually removing them naturally over time. Most patients will see an immediate improvement in appearance, as the sclerosant changes the color of the vein once introduced. Multiple “touch -up” visits are usually required.
Cost of Sclerotherapy in Westlake, OH
No two sclerotherapy treatments are exactly alike. For an accurate estimate of the cost of your treatment, please book a personal consultation with us at your earliest convenience. Don’t live with the embarrassment and discomfort of spider veins or varicose veins any longer. Get professional advice about venous disease from one of Ohio’s leading vascular surgeons. Contact (440) 641-0433 to speak to our booking team. Dr. Naar can craft a vein treatment plan that will help you get the results you want, improve your quality of life, and rid you of unsightly spider veins!
References
- Sandean DP, Winters R. Spider Veins. PubMed. Published 2022. https://www.ncbi.nlm.nih.gov/books/NBK563218/
- Robles-Tenorio A, Lev-Tov H, Ocampo-Candiani J. Venous Leg Ulcer. PubMed. Published 2021. https://www.ncbi.nlm.nih.gov/books/NBK567802/
- Nakano LC, Cacione DG, Baptista‐Silva JC, Flumignan RL. Treatment for telangiectasias and reticular veins. The Cochrane Database of Systematic Reviews. 2017;2017(7). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6483333/
- Zegarra TI, Tadi P. CEAP Classification Of Venous Disorders. PubMed. Published 2022. https://www.ncbi.nlm.nih.gov/books/NBK557410/
- Worthington-Kirsch, R. L. (2005). Injection Sclerotherapy. Seminars in Interventional Radiology, 22(3), 209–217. https://doi.org/10.1055/s-2005-921954