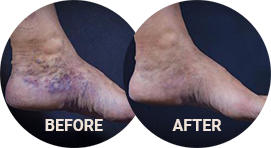
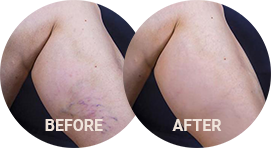
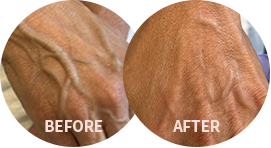
For most people, varicose veins are a benign or cosmetic condition causing few symptoms or other health issues. Oftentimes symptoms of venous disease can go unnoticed. The redundancies of the circulatory system usually find a way to supply blood to all tissue. Venous ulcers occur when the poorly functioning valves inside your veins interfere with normal blood flow to the point that veins can no longer adequately circulate blood. It becomes like a waterfall. Tissue can start retaining fluid and dying from lack of oxygen and nutrients.
How Venous Ulcers Begin
Because veins normally operate with a lower blood pressure than the arterial system, vein walls have valves that open to let blood pass, while closing to prevent backflow. This is particularly important in your legs, where blood returning to the heart usually faces an uphill climb. When these veins begin to fail, blood can pool, and pressure can build up beyond the capabilities of the venous system.
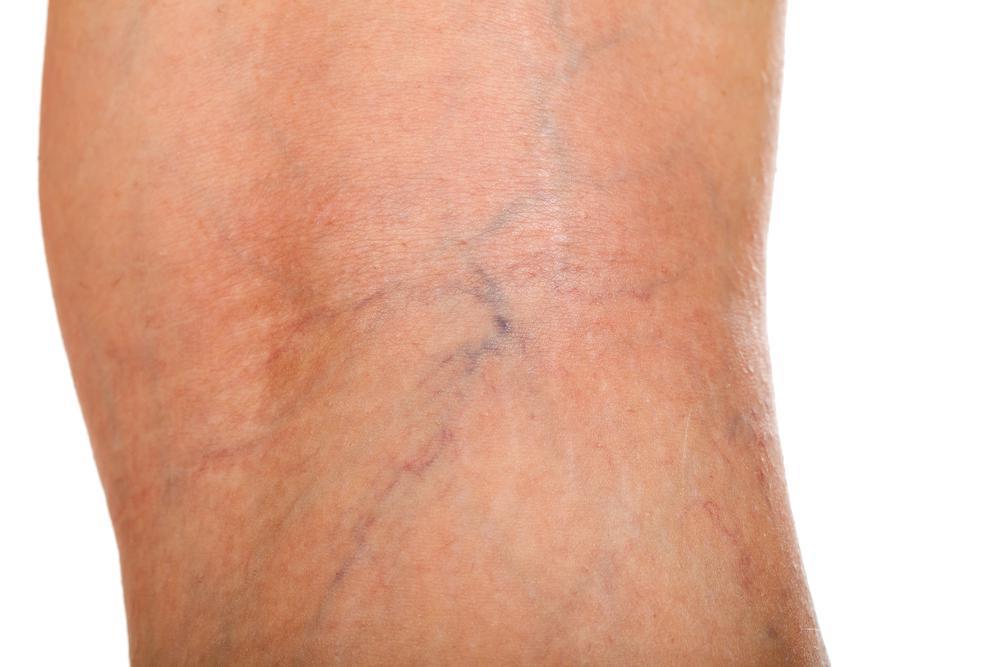
The twisting bulges of varicose veins are the usual visual sign of failing valves. Simply having varicose veins doesn’t mean that you’ll develop venous ulcers though. These usually begin when you have a break in the skin, usually on the lower leg near an ankle. The increase in local blood pressure can delay ordinary healing. The skin break may turn from a minor problem into an ulcer, which can be much more serious.
Symptoms of Venous Ulcers
You may first feel an itching or burning sensation in the area of an ulcer. The skin in the area may feel dry or show signs of a rash. There may also be brown color changes, and the sore may start to leak fluid that has a strong, foul smell. Once the venous ulcer starts, there’s a risk it will become infected, usually revealed by increased pain and redness in the area, as well as pus leakage and an accompanying fever.
Treatment ranges from rest and elevation of the affected leg, compression stockings or bandages, antibiotics if the ulcer is infected, and surgery, which may be needed to improve circulation and prevent recurrence.
Risk Factors for Venous Ulcers
Having diabetes is a major risk factor for developing venous ulcers. Changes to your blood vessels due to high glucose levels leave them vulnerable to conditions that form ulcers. These changes can reduce blood flow as well as cause nerve problems that prevent you from feeling the effects of ulcers until the later stages. Venous ulcers can, in extreme cases, lead to limb amputation.
Congestive heart failure also creates challenges for your circulatory system, which can contribute to venous ulcers. The same holds true for other disorders of blood vessels such as peripheral vascular disease and deep vein thrombosis. All factors that contribute to these conditions also raise your risk of developing venous ulcers.
Some of the more common contributors to venous leg ulcers include:
- High body mass index
- Hypertension
- Kidney failure
- Pregnancy and other conditions affecting female hormone levels
- Tobacco use
- The process of aging
- Sitting or standing for long periods of time
- Family history of circulatory issues
If you’re suffering from venous ulcers, or if you have several risk factors and want to ensure you don’t develop ulcers in future, contact Dr. Naar at Premier Vein Clinic for a comprehensive evaluation. You can reach the office by phone or by using the appointment request tool on the website.
There’s no need to endure the discomfort of venous leg ulcers. Contact us today.