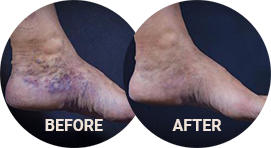
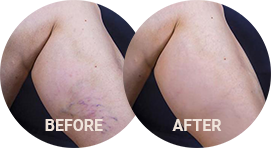
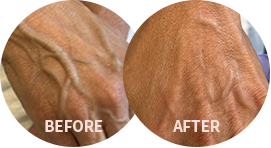
Phlebitis, also known as venitis, is the inflammation and thickening of the wall of a vein caused by a blood clot, a mechanical injury, a chemical injury, or an infection. Superficial veins can become inflamed due to internal or external forces, and may occur in varicose veins. There are also many other factors that increase the risk of developing phlebitis, including age, pregnancy, medications, and obesity. Inflammation can also occur in deeper veins due to blood clots, known as deep vein thrombosis (DVT).
Venous inflammation can cause unwanted side-effects including pain, itching, and redness. Where the vein is infected by bacteria, patients may also experience a low-grade fever. These can be both uncomfortable and inconvenient, reducing quality of life and decreasing mobility.
Board-certified vascular surgeon Dr. David Naar provides comprehensive phlebitis management and treatment for patients in Westlake, Ohio. At Premier Vein Clinic, you can find relief from phlebitis, venous disease, varicose veins, and DVT. To schedule a consultation with us, call our office at (440) 641-0433 or fill out an inquiry form on our website.
Contents
About Venous Inflammation
Veins play a vital role in the cardiovascular system, particularly in the feet and legs. The heart is not powerful enough to work against gravity alone. So, these tubular structures direct blood flow back to the heart through a system of one-way valves. However, when our veins are damaged, or not working well, many problems can occur, which can affect our daily lives and lead to further complications.
Superficial phlebitis (ST) occurs near the surface of the skin. It primarily affects patients who already have varicose veins. It usually occurs in the lower legs, but it may affect other areas of the body, such as the arms. A vein can become inflamed for many reasons, particularly when blood clots form. This causes inflammation, swelling, and discomfort. This is known as thrombophlebitis. It can disrupt blood flow, and alter the physical shape of the vein itself, as can mechanical injury, such as from a large IV cannula, a chemical injury from the agent that is being infused, or from bacteria that have caused an immune response in the body. But how do you know if you have phlebitis? And what are the most common symptoms?
Symptoms of Phlebitis
Common signs of phlebitis include:
- Pain, Tenderness
- Lumps in Varicose Veins
- Skin Redness
- Sensation of Warmth
- Visible Bulging
- May Have No Symptoms
Who is at Risk?
Although the walls of our veins are resilient, phlebitis can materialize for many reasons. At particular risk are those who frequently require the placement of IVs. Some studies also suggest that women are more likely to develop phlebitis. Similarly, age is a significant factor. One survey of nurses found that obvious signs of phlebitis were present in approximately 50% of their patients over the age of 60. (1)
The most common risks for developing phlebitis are:
- Smoking
- Varicose Veins
- Oral Contraceptive Use
- Being Bedridden/Immobile
- Pregnancy
- Hormone Replacement Therapy
- Cancer
- Surgical lymph node removal
- Bleeding Disorders
- History of Blood Clots
- Sedentary Lifestyle
- Intravenous drug use
Studies show that between 6 to 36% of patients with superficial phlebitis develop DVT. In the most severe cases, this can lead to pulmonary embolism. (2)
Types of Phlebitis
Mechanical Phlebitis
Blood, fluid, and medication infusions are often required for the treatment of common medical conditions. Therefore, patients who undergo frequent IV infusions may run a higher risk of ST. An intravenous indwelling needle, or trocar, is placed into a vein in IV infusion. However, if a needle that is too large for a vein is inserted, it may cause damage that leads to phlebitis. Similarly, if trauma occurs to the vein while it is catheterized, such as pulling, this may also lead to mechanical phlebitis. This type of phlebitis is described by some patients as particularly uncomfortable.(3)
Chemical Phlebitis
Normal blood pH is between 7.35 and 7.45. Chemical phlebitis can occur when the fluid administered through the IV line irritates the vein due to being too acidic or too alkaline, disrupting the pH balance. This can be caused by incorrectly diluted medication or an incorrect infusion rate into the body.
Infective Phlebitis
Infective phlebitis, also known as septic thrombophlebitis, is caused by the introduction of pathogens into the vein. This can be due to IV catheter contamination, skin breakdown, or a non-venous structure within the body. The most common organism in cases of infective phlebitis is staphylococcus aureus bacteria, although other pathogens such as viruses and pathogens can cause it. (4)
Phlebitis Severity Scale & Management
Phlebitis has four grades of severity:
Grade 1 – Reddening around the puncture site, with or without local pain.
Grade 2 – Puncture site pain with reddening and/or swelling and hardening.
Grade 3 – Puncture site pain with reddening, hardening and a palpable venous cord.
Grade 4 – Puncture site pain site with reddening, hardening and a palpable venous cord that is greater than 1 cm (0.39 in.), with purulent discharge (pus). (4)
Treatments for Phlebitis
Phlebitis management takes many forms. Depending on your individual treatment plan, Dr. Naar may suggest conservative management or surgery.
Elevate the Limb – Dr. Naar may suggest elevating the affected limb when you are at rest to help reduce swelling. Using pillows or cushions to raise it to a comfortable position when sitting or sleeping.
Wear Compression Stockings – Compression stockings are designed to encourage blood flow, reduce swelling, and manage discomfort. Patients should wear them in the daytime only.
Apply a Warm, Moist Compress – Warmth brings blood closer to the surface. It also soothes the area.
Non-Steroidal Anti-Inflammatory Medications (NSAIDs) – NSAIDs such as aspirin, ibuprofen (Advil), or naproxen (Aleve) help to reduce pain. They may also help to lower the risk of thrombophlebitis spreading to deeper veins and decreasing recurrence of the condition.
Anticoagulant Medications – Where superficial phlebitis has developed into DVT, Dr. Naar may recommend treatment with anticoagulant medications such as Xarelto, Warfarin or Eliquis. These medications slow down the body’s clot-making processes, therefore reducing the risk of further clots developing.
In some cases, phlebitis will resolve on its own. However, if your symptoms persist, you may wish to seek further treatment. In more severe cases of phlebitis, and if there is a higher risk of a patient developing DVT, Dr. Naar may recommend a surgical procedure to address the affected vein.
Surgical management may include:
- Excision of the problem vein
- Surgical vein closure (sclerotherapy)
- Clot removal (surgical thrombectomy)
Many people experience phlebitis and varicose veins. In these cases, Dr. Naar may suggest a combination therapy plan that involves both conservative management and surgical procedures to alleviate discomfort and mitigate further instances of the condition.
Candidates for Phlebitis Treatment
Most patients experiencing the symptoms of phlebitis, or those that suspect it, are suitable candidates for phlebitis treatment at Premier Vein Clinic. Finding out exactly what is wrong can significantly impact quality of life and comfort levels. You can do so by booking a personal consultation with Dr. Naar to diagnose the condition and its severity. After this, he will formulate a treatment plan that will be most beneficial for your long-term health goals.
Personal Consultation
Dr. Naar determines phlebitis and DVT intervention plans with physical examination. He may also require blood tests, and ultrasound. At your personal consultation, he will inspect the veins in question and ask you about the symptoms you have been experiencing to determine the best course of treatment for you.
Cost of Phlebitis Treatment in Westlake, OH
The cost of your treatment will vary according to the treatment plan designed for you personally by Dr. Naar. For further information about Premier Vein Clinic, and to book an individual consultation for a phlebitis assessment, call (440) 641-0433.
FAQ
Is phlebitis the same as DVT?
Phlebitis is swelling and inflammation in a vein or multiple veins. Without proper management, superficial phlebitis may migrate to deeper veins and cause further complications. Superficial phlebitis affects the veins that are closest to the surface of the skin, whereas deep vein thrombosis (DVT) affects deeper veins. Phlebitis that occurs in deep veins is known as thrombophlebitis.
How do I know if I have phlebitis?
Phlebitis usually affects the legs. It is characterized by redness, swelling, and discomfort in the area of concern. Patients may also experience warmth, and the vein may appear rope-like through the skin.
If I have varicose veins, do I have phlebitis?
Phlebitis is a frequent complication of varicose veins, but this is not always the case. Mechanical phlebitis may also be caused by IV insertion, an adverse reaction to the fluid being infused, or infection.
References
- Milutinović, D., Simin, D., & Zec, D. (2015). Risk factor for phlebitis: a questionnaire study of nurses’ perception. Revista Latino-Americana de Enfermagem, 23(4), 677–684. https://doi.org/10.1590/0104-1169.0192.2603
- Czysz, A., & Higbee, S. L. (2020). Superficial Thrombophlebitis. PubMed; StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK556017/
- Lu, Y., Hao, C., He, W., Tang, C., & Shao, Z. (2017). Experimental research on preventing mechanical phlebitis arising from indwelling needles in intravenous therapy by external application of mirabilite. Experimental and Therapeutic Medicine. https://doi.org/10.3892/etm.2017.5347
- Urbanetto, J. de S., Peixoto, C. G., & May, T. A. (2016). Incidence of phlebitis associated with the use of peripheral IV catheter and following catheter removal. Revista Latino-Americana de Enfermagem, 24(0). https://doi.org/10.1590/1518-8345.0604.2746